Table of Contents
Side effects of causes restless leg syndrome
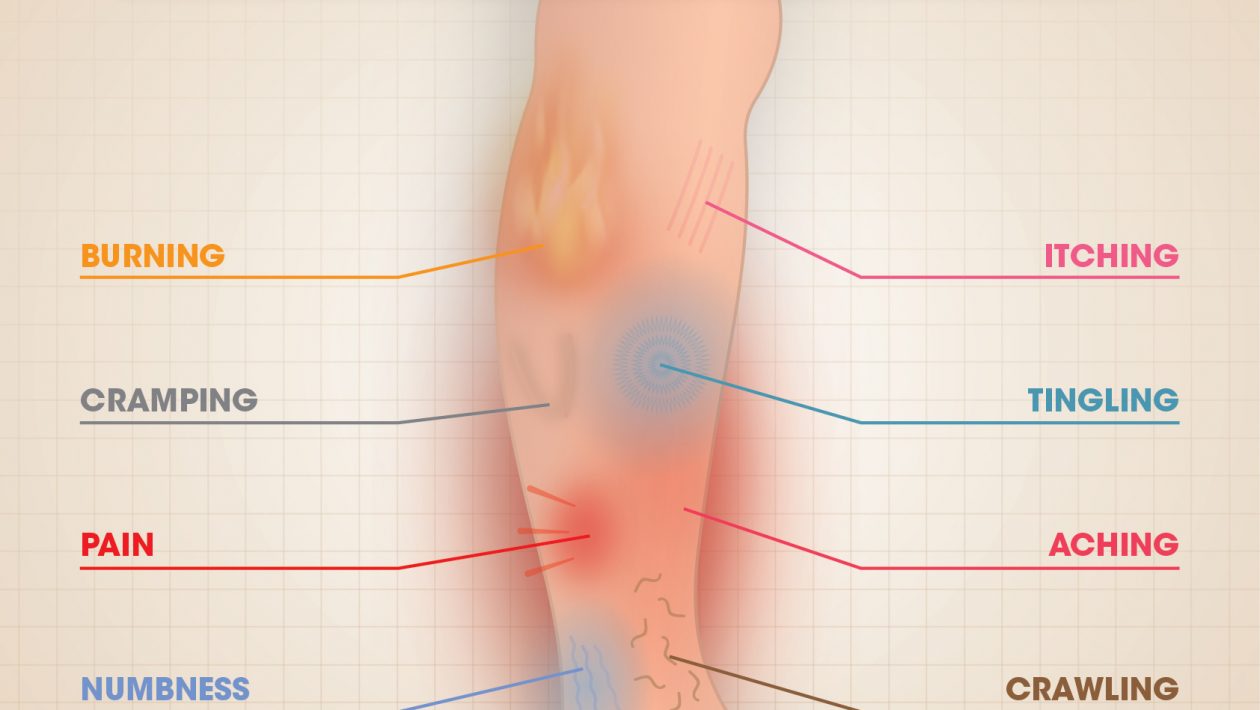
The main side effect of causes restless leg syndrome condition is the incredible desire to move the legs.
It also produces an unpleasant slippery or slippery sensation on the feet, calves, and thighs.
In the evening or early evening, this feeling is usually more frightening. By the way, the arm will also be affected.
Nervous leg disorders are also associated with a compulsory snapping of the legs and arms, called incidental resting appendage development (PLMS).
A few people rarely show signs of leg discomfort, while others are consistent.
The form of expression can vary from mild to extreme. In extreme cases, anxious leg conditions can be disturbing and disturb the individual’s daily exercise.
What causes restless leg syndrome?
In most cases, there is no apparent cause for leg discomfort.
This is called idiopathic or essential anxiety disorder and can occur in the family.
Some neurologists (experts who treat diseases that affect the sensory system) accept that the manifestations of anxiety and leg disorders may be related to how the body processes a substance called dopamine.
Dopamine controls muscle development and may be responsible for compulsory leg development related to leg discomfort.
Time and time again, irritable leg diseases are caused by fundamental medical problems, such as iron deficiency or pale kidneys, or disappointing kidneys. This is called optional anxiety disorder.
There is also a link between leg anxiety and pregnancy. Although this is not satisfactory in practice, 1 in 5 pregnant women will experience symptoms within the last three months of pregnancy.
In this case, usually, after the wife becomes pregnant, the causes restless leg syndrome
Leg discomfort (RLS) is a condition that usually causes your legs to turn sharply due to awkward feelings. It usually occurs at night or night, when you are sitting or resting. Movement helps to tilt, by the way.
Leg anxiety disorder (also known as Willis-Ekbom disease) can start at any stage of life and worsen significantly with age. It interferes with rest, and rest interferes with daily exercise.
Necessary self-care steps and lifestyle changes may help alleviate the indications. Medications can also help many patients with RLS.
Your PCP will record your clinical history and ask for a description of your side effects. The conclusion of RLS depends on the rules established by the International Research Group on Restless Legs Syndrome:
Your legs are firm and often eye-catching, and they usually move due to awkward feelings.
When resting (such as sitting or sleeping), your performance begins or deteriorates.
Exercise (for example, walking or stretching) will not reduce your performance ultimately or accidentally.
In the evening, your performance is even more terrifying.
The performance cannot be clarified by other clinical or social conditions alone.
Your primary care physician may direct physical and neurological examinations. A blood test may be required, especially for iron deficiency, to rule out other possible indications.
Moreover, your PCP may imply that you are a trained professional. This may include a short stay in a rest center. If you suspect other rest problems, such as alleged apnea, the expert can consider your rest. In any case, determining RLS usually does not require further research.
treatment
Occasionally treating hidden conditions, such as iron deficiency, can significantly reduce the signs of RLS. Correcting iron deficiency may include taking iron supplements orally or intravenously. Nevertheless, only after clinical management and your primary care doctor have checked your blood iron levels, iron supplements should be taken.
If you have RLS without related conditions, treatment will revolve around lifestyle changes. If these features are not powerful, your primary care doctor may approve these prescriptions.
medicine
You can use some medicines prescribed by doctors, most of which are used to treat different diseases, reducing your legs’ anxiety. These include:
Drugs that enlarge dopamine in the brain. These prescriptions will affect the level of compound express dopamine in your brain. The Food and Drug Administration has approved ropinirole (Requip), rotigotine (Neupro), and pramipexole (Mirapex) for the treatment of moderate to severe RLS.
The instant symptoms of these drugs are usually mild, accompanied by discomfort, dizziness, and fatigue. Nevertheless, they can also cause drive control problems, such as enthusiastic betting and daytime fatigue.
Drugs that affect calcium channels. Certain medications, such as gabapentin (Neurontin, Gralise), gabapentin enacarbil (Horizant), and pregabalin (Lyrica), are useful for individual patients with RLS.
Drug. Opioids can relieve mellow symptoms to severe symptoms, but they may be irresistible when used in high doses. Some models include tramadol (Ultram, ConZip), codeine, oxycodone (Oxycontin, Roxicodone, etc.), and hydrocodone (Hysingla ER, Zohydro ER).
Muscle relaxants and sleeping pills. These medicines can help you rest better in the evening, but they will not eliminate leg discomfort and may cause laziness during the day. If there is no other treatment to relieve, these prescriptions can usually be used.
You and your PCP may need some preliminary preparations to find the right medicine or mixture of drugs that best suit you.
Remind prescription
Some dopamine drugs that can relieve your RLS effects for some time are not sufficient, or you find that your symptoms return a day ago or include your arms. This is called growth. Your primary care doctor can substitute another medicine to solve the problem.
Most drugs approved for the treatment of RLS are not recommended during pregnancy. Taking all factors into consideration, your PCP may develop self-care strategies to reduce symptoms. In any case, if you feel incredibly annoying during the last three months, your primary care doctor may support the use of specific medications.
Certain drugs may worsen the side effects of RLS. These drugs include some antidepressants, some antipsychotics, some enemies of tranquilizers, and some cold and allergy medicines. Your primary care physician may recommend that you avoid these drugs. Nonetheless, if you do not have many opportunities to take these drugs, please discuss adding drugs to treat RLS with your primary care doctor.
Lifestyle and family therapy
Making necessary lifestyle changes can help reduce the side effects of RLS:
Try showers and back massages. Taking a hot bath and kneading your legs can relax the muscles.
Apply warm or cool packaging. The use of warm or cold, or the exchange of the two, may reduce the sensation of your appendix.
Set up good rest cleanliness. Tiredness usually destroys the signs of RLS, so it is essential to maintain good rest hygiene. It is best to keep cool, calm, and be satisfied with the do-do climate; the hay rises at the same time every day; in any case, you have to rest for seven hours a day.
Exercise. Performing moderate standard exercise may calm the performance of RLS, but excessive effort or more than a day’s non-profit point may increase the indications.
Stay away from caffeine. Reducing caffeine from time to time may help discomfort the legs. Try to stay away from caffeinated items for half a month, including chocolate, espresso, tea, and soda, to check if this makes a difference.
Consider using foot covers. Foot care is especially suitable for patients with RLS. It can put pressure on your feet and help reduce side effects.
Adaptation and support
RLS is generally a long-term condition. Using RLS includes creating adaptation techniques that suit you, for example,
Tell others about your situation. Sharing data about RLS will help your relatives, companions, and colleagues to understand better when you step into the lobby, stay at the back of the theater, or stroll to the water dispenser during the typical day of the day.
Try not to oppose your development needs. If you try to suppress the tendency to move, you may find that your performance deteriorates.
Keep a diary of rest. Monitor the drugs and methods that help or thwart the fight against RLS, and provide this data to your primary care physician.
Stretch and wipe back. Start and end the day with extended exercises or delicate back scrubs.
Seek help. The nursing team combines relatives and individuals with RLS. By being interested in gatherings, your experience can help not only you but also other people.
Plan your arrangement
If you have side effects of RLS, please meet with your primary care doctor. After a basic assessment, the relevant person may suggest an expert (Eurosystem expert) or other subject matter expert who spends a lot of time in sensory system conditions.
Here are some data to help you prepare for the arrangement.
what can you do
Record your indications, including when they started and when they usually occur.
Record critical clinical data, including the different conditions you are in and any solutions or over-the-counter medications you are taking, including nutrients and enhancers. Also, please be aware of the existence of past RLS in your family.
Bring relatives or companions. People traveling with you may recall data you missed or failed to remember.
Record the inquiry with your primary care doctor.
Some necessary inquiries about RLS to your PCP include:
What is the most likely cause of my signs and indications?
Are there other potential reasons?
What test do I need?
What alternative treatments are available for this situation?
I have other diseases. How can I best supervise them together?
Which self-care steps can improve my performance?
Do you have any guidance materials that I can get? Which website do you recommend?
Where can I find a care team for patients with RLS?
What’s stored in PCP
Your PCP may ask you various queries, including:
Do you have a strong tendency to move your feet?
What words do you use to describe your performance?
Do side effects start when sitting or resting?
In the evening, are your side effects more regrettable?
Improve?
Have you been told to kick, shake or move your legs under any circumstances when you hit?
Do you often have difficulty falling or staying unconscious?
It is safe to say that you are exhausted during the day?
Does anyone else in your family have leg anxiety?
How much caffeine do you have every day?
What is your usual exercise routine?
It can be said with certainty that you are at risk of low iron due to restricted meat in your diet, frequent blood draws, or blood misfortunes caused by new medical procedures?
What can you do at the same time?
For instructions, please try:
Reduce or remove caffeine, alcohol, and tobacco
Rub your legs while taking a hot bath.
Risk factors causes restless leg syndrome
RLS can be creative at any stage of life, in any case, in youth. As we age, this problem becomes more common, and women are more common than men.
RLS is usually not recognized as a real clinical risk. However, sometimes it changes with different conditions, for example,
Limbic neuropathy. Sometimes due to persistent infections, such as diabetes and alcohol abuse, damage your grip and nerves in your feet.
Lack of iron. Indeed, even if there are no defects, iron deficiency can cause or worsen RLS. Suppose your experience is full of a history of infiltration from the stomach or inside, experiencing a heavy female period, or donating blood over and over again. In that case, you may be suffering from iron deficiency.
The kidneys are disappointed. If you have the chance of kidney disappointment, you may also often lack iron and look pale. When the kidneys are not working correctly, the iron storage in the blood decreases. Such changes and different changes in human science may cause or destroy RLS.
Spinal cord condition. Spinal cord injury due to injury or injury has been associated with RLS. Calming the spinal cord, for example, the square of the spine also increases the risk of RLS.
inconvenience causes restless leg syndrome
Although RLS does not indicate other real symptoms, the side effects may change from being barely annoying to diminishing. Many people with RLS think it is difficult to fall off or remain unconscious.
Severe RLS can lead to a severe decline in the quality of life and can lead to grief. Insufficient sleep can cause extreme daytime sluggishness, but RLS may snooze.